Clinical case
Published in spanish Científica Dental Vol. 17. Nº 1. 2020 www.cientificadental.es
Atrophic posterior maxilla: sinus elevation with lateral approach Vs. Extra-short implants. Clinical case with eight years of follow-up
Vertical bone loss in the posterior maxillary sectors is a frequent occurrence after tooth extraction. These areas can often be rehabilitated using regeneration techniques or by opting for a more conservative approach with short implants.
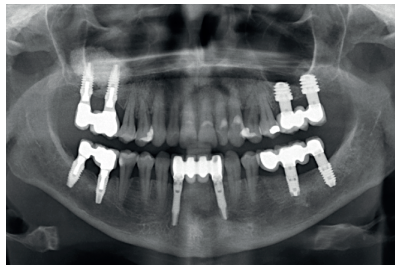
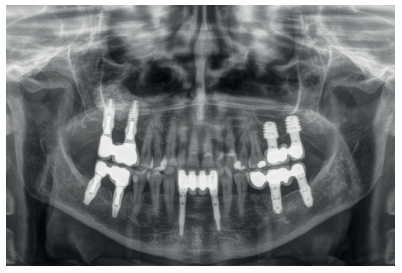
The present clinical case shows bilateral rehabilitation with two different techniques: sinus lift and the insertion of short implants, with a follow-up of 8 years where both techniques have achieved equally predictable results.
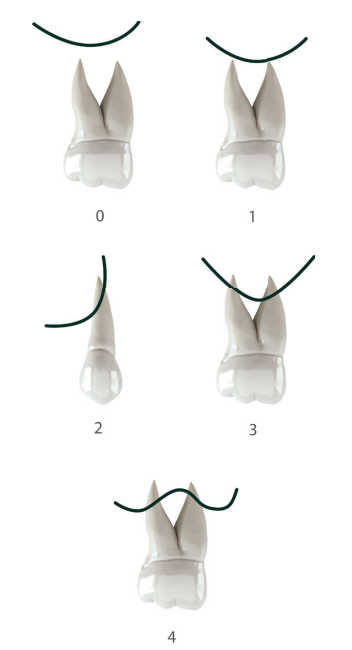
Approaching the posterior sectors of the maxilla with extreme resorption is a common situation in dental practice. The loss of antral teeth produces pneumatisation of the maxillary sinus, which progressively occupies the space corresponding to the dental roots, in some cases leading to complete atrophy and in a residual bone height of 1-2 mm aft er the dental socket heals. This pneumatisation occurs over ti me aft er tooth extraction, but is unpredictable in terms of quanti ty and speed, and appears to be slightly related to the type of relationship that occurs between the apex and the sinus. This relationship was described by Sharan and Madjar in 2008, who established a classification with greater pneumatisation is expected in its types 3 and 4 (Figure 1)1 .
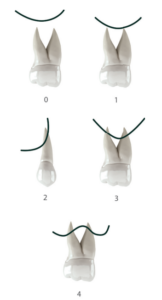
the floor of the maxillary sinus.
Type 0: The root is not in contact with the sinus cortex.
Type 1: The sinus cortex is less convex and makes slight contact with the upper area of the root apex.
Type 3: The sinus cortex describes a curve of lower convexity and the apices of the roots of the antral teeth project into the sinus.
Type 4: The sinus cortex is less concave surrounding the apices
of the antral teeth, and there may be a slight prolongation of the root apices inside the sinus.
Until the arrival of short and extra-short implants, the only alternative treatment in these cases was sinus elevation (laterally or transcrestally), and there were different techniques and procedures for this. The attempt was to gain the lost bone volume and the subsequent insertion of conventional length implants at this level2-6.
The development of short implants and the entire technique for their use sometimes allows the insertion of implants in large posterior vertical atrophies of the maxilla, avoiding sinus elevations.
Nowadays, most authors accept short implants to be those with a length less than 8.5 mm, although there are many cases of lengths well below this figure7-9. Extra-short implants, meanwhile, have more variation in terms of their classification; although the latest articles published consider extra-short implants to be those with a length less than 7 mm10-12. These shorter implants mean less morbidity for pati ents, at the same ti me as it is now possible to rehabilitate pati ents who may refuse to have additional techniques performed. These are sinus elevation and even more complex techniques which may be contraindicated in these pati ents for different medical reasons13-17. These short and extra-short implants can be inserted in the atrophic areas of the maxilla directly without displacement of the lower sinus cortex and without therefore having to manoeuvre the maxillary sinus. The main surgical challenge with this technique is to achieve implant stability, since generally in these cases we are faced with little remaining bone height and with high porosity18-22. Therefore, the establishment of a careful surgical protocol based on drilling into the receptor bed depending on its condition is key to the success of these treatments13-17.
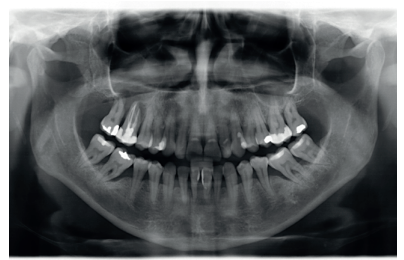
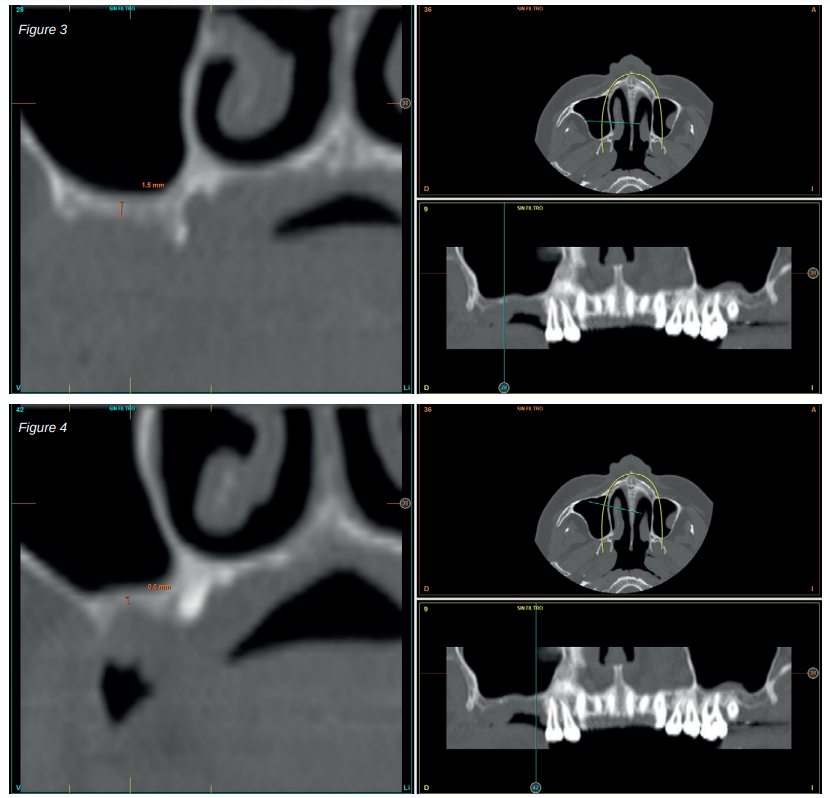
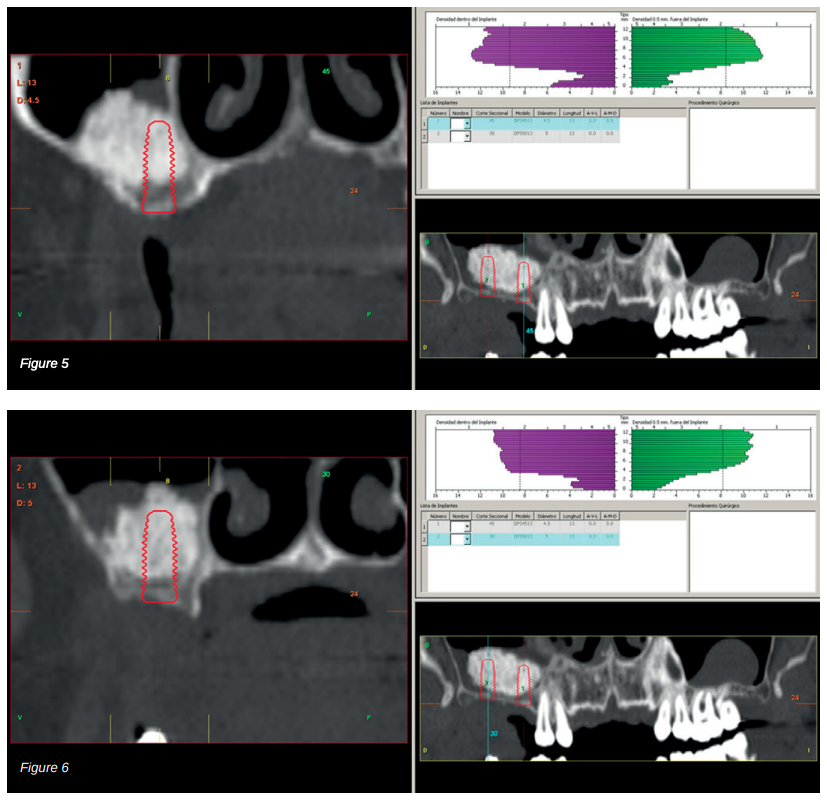
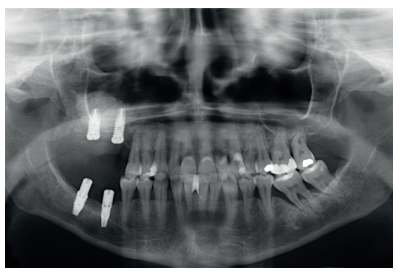
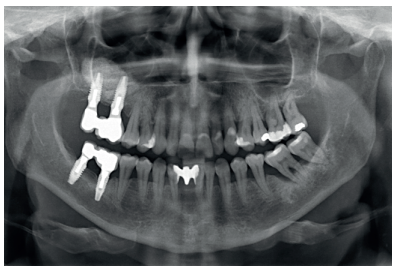
The clinical case described is of a patient receiving both procedures: extra-short implants inserted directly into one maxillary quadrant and a sinus lift with conventional length implants in the other quadrant. The evolution of both treatments in the same patient was able to be observed over eight years.
Sharan A, Madjar D. Maxillary sinus pneumatization following extractions: a radiographic study. Int J Oral Maxillofac Implants 2008; 23(1):48-56.
Correia F, Pozza DH, Gouveia S, Felino A, Faria E, Almeida R. The applications of regenerative medicine in sinus lift procedures: A systematic review. Clin Implant Dent Relat Res 2018; 20:229-242.
Cho YS, Chong D, Yang SM, Kang B. Hydraulic Transcrestal Sinus Lift: Different Patterns of Elevation in Pig Sinuses. Implant Dent 2017; 26:706-10.
Li Y, Hu P, Han Y, Fan J, Dong X, Ren H, Yang C, Shi T, Xia D. Ex vivo comparative study on three sinus lift tools for transcrestal detaching maxillary sinus mucosa. Bioengineered 2017; 4(8):359-66.
Silva LD, de Lima VN, Faverani LP, de Mendonça MR, Okamoto R, Pellizzer EP. Maxillary sinus lift surgery-with or without graft material? A systematic review. Int J Oral Maxillofac Surg 2016; 45:1570-6.
Borgonovo AE, Vitaliano T, Medagliani P, Bianchi A, Re D. Crestal sinus lift by using a mini-invasive procedure: a case series. Minerva Stomatol 2016; 65:107-17.
Esfahrood ZR, Ahmadi L, Karami E, Asghari S. Short dental implants in the posterior maxilla: a review of the literature. J Korean Assoc Oral Maxillofac Surg 2017; 43:70-6.
Lemos CA, Ferro-Alves ML, Okamoto R, Mendonça MR, Pellizzer EP. Short dental implants versus standard dental implants placed in the posterior jaws: A systematic review and meta-analysis. J Dent 2016; 47:8-17.
Cannizzaro G, Felice P, Leone M, Viola P, Esposito M. Early loading of implants in the atrophic posterior maxilla: lateral sinus lift with autogenous bone and Bio-Oss versus crestal mini sinus lift and 8-mm hydroxyapatite-coated implants: a randomised controlled clinical trial. Eur J Oral Implantol 2009; 2:25-38.
Gürlek Ö, Kaval ME, Buduneli N, Nizam N. Extra-short implants in the prosthetic rehabilitation of the posterior maxilla. Aust Dent J 2019; 64:353-8.
Calvo-Guirado JL, Morales-Meléndez H, Pérez-Albacete Martínez C, Morales-Schwarz D, Kolerman R, Fernández-Domínguez M, Gehrke SA, Maté-Sánchez de Val JE. Evaluation of the surrounding ring of two different extra-short implant designs in crestal bone maintanence: A histologic study in dogs. Materials (Basel). 2018 6;11(9) doi: 10.3390/ma11091630.
Pommer B, Mailath-Pokorny G, Haas R, Buseniechner D, Millesi W, Fürhauser R. Extra-short (< 7 mm) and extra-narrow diameter (< 3.5 mm) implants: a meta-analytic literature review. Eur J Oral Implantol 2018;11 Suppl 1: S137-S146.
Anitua E, Alkhraisat MH. 15-year follow-up of short dental implants placed in the partially edentulous patient: Mandible Vs maxilla. Ann Anat 2019; 222:88-93.
Hernández-Marcos G, Hernández-Herrera M, Anitua E. Marginal bone loss around short dental implants restored at implant level and with transmucosal abutment: A retrospective study. Int J Oral Maxillofac Implants 2018; 33:1362-7.
Anitua E, Piñas L, Escuer-Artero V, Fernández RS, Alkhraisat MH. Short dental implants in patients with oral lichen planus: a long-term follow-up. Br J Oral Maxillofac Surg 2018; 56:216-20.
Anitua E. Immediate loading of short implants in posterior maxillae: Case series. Acta Stomatol Croa 2017; 51:157-62.
Anitua E, Flores J, Flores C, Alkhraisat MH. Long-term outcomes of immediate loading of short implants: A controlled retrospective cohort study. Int J Oral Maxillofac Implants 2016; 31:1360-6.
Anitua E, Tapia R, Luzuriaga F, Orive G. Influence of implant length, diameter, and geometry on stress distribution: a finite element analysis. Int J Periodontics Restorative Dent 2010; 30:89-95.
Anitua E. A new approach for treating peri-implantitis: Reversibility of osseointegration. Dent Today 2016; 35:130-1.
Anitua E, Murias-Freijo A, Alkhraisat MH. Conservative implant removal for the analysis of the cause, removal torque, and surface treatment of failed nonmobile dental implants. J Oral Implantol 2016; 42:69-77.
Villarinho EA, Triches DF, Alonso FR, Mezzomo LAM, Teixeira ER, Shinkai RSA. Risk factors for single crowns supported by short (6-mm) implants in the posterior region: A prospective clinical and radiographic study. Clin Implant Dent Relat Res 2017; 19:671-80.
Esfahrood ZR, Ahmadi L, Karami E, Asghari S. Short dental implants in the posterior maxilla: a review of the literature. J Korean Assoc Oral Maxillofac Surg 2017; 43:70-6.
Lemos CA, Ferro-Alves ML, Okamoto R, Mendonça MR, Pellizzer EP. Short dental implants versus standard dental implants placed in the posterior jaws: A systematic review and meta-analysis. J Dent 2016; 47:8-17.
Anitua E, Alkhraisat MH, Piñas L, Orive G. Efficacy of biologically guided implant site preparation to obtain adequate primary implant stability. Ann Anat 2015; 199:9-15.
Tatum H. Maxillary and sinus implant reconstructions. Dent Clin North Am 1986; 30:1207-29.
Beretta M, Poli PP, Grossi GB, Pieroni S, Maiorana C. Long-term survival rate of implants placed in conjunction with 246 sinus floor elevation procedures: results of a 15-year retrospective study. J Dent 2015; 43:78-86.
Viña-Almunia J, Peñarrocha-Diago M, Peñarrocha-Diago M. Influence of perforation of the sinus membrane on the survival rate of implants placed after direct sinus lift. Literature update. Med Oral Patol Oral Cir Bucal 2009;14: E133-6.
Tolentino da Rosa de Souza P, Binhame Albini Martini M, Reis Azevedo-Alanis L. Do short implants have similar survival rates compared to standard implants in posterior single crown?: A systematic review and meta-analysis. Clin Implant Dent Relat Res 2018; 20(5):890-901.
Summers RB. A New Concept in maxillary implant surgery: the osteotome technique. Compendium 1994;15:154–6.
Cavicchia F, Bravi F, Petrelli G. Localized augmentation of the maxillary sinus floor through a coronal approach for the placement of implants. Int J Periodontics Restorative Dent 2001; 21:475-85.
Del Fabbro M, Corbella S, Weinstein T, Ceresoli V, Taschieri S. Implant survival rates after osteotome-mediated maxillary sinus augmentation: a systematic review. Clin Implant Dent Relat Res 2012; 14(Suppl 1): e159-68.
Petrungaro PS, Kurtzman GM, Gonzales S, Villegas C. Zygomatic implants for the management of severe alveolar atrophy in the partial or completely edentulous maxilla. Compend Contin Educ Dent 2018; 39:636-45.
Faot F, Thomé G, Bielemann AM, Hermann C, Melo AC, Padovan LE, de Mattias Sartori IA. Simplifying the treatment of bone atrophy in the posterior regions: Combination of zygomatic and wide-short implants-a case report with 2 years of follow-up. Case Rep Dent 2016; 2016:5328598.
Bastos AS, Spin-Neto R, Conte-Neto N, Galina K, Boeck-Neto RJ, Marcantonio C, Marcantonio E, Marcantonio E Jr. Calvarial autogenous bone graft for maxillary ridge and sinus reconstruction for rehabilitation with dental implants. J Oral Implantol 2014; 40:469-78.
Pistilli R, Signorini L, Pisacane A, Lizio G, Felice P. Case of severe bone atrophy of the posterior maxilla rehabilitated with blocks of equine origin bone: histological results. Implant Dent 2013; 22: 8-15.
Gastaldi G, Felice P, Pistilli R, Barausse C, Trullenque-Eriksson A, Esposito M. Short implants as an alternative to crestal sinus lift: a 3-year multicentre randomised controlled trial. Eur J Oral Implantol 2017; 10:391-400.
D’Amato S, Borriello C, Tartaro G, Itro A. Maxillary sinus surgical lift. Summers’ technique versus lateral surgical approach. Minerva Stomatol 2000; 49:369-81.