Systematic review
Published in spanish Científica Dental Vol. 18. Nº 2. 2021 www.cientificadental.es
Use of particulate dentin in alveolar preservation procedures: a systematic review
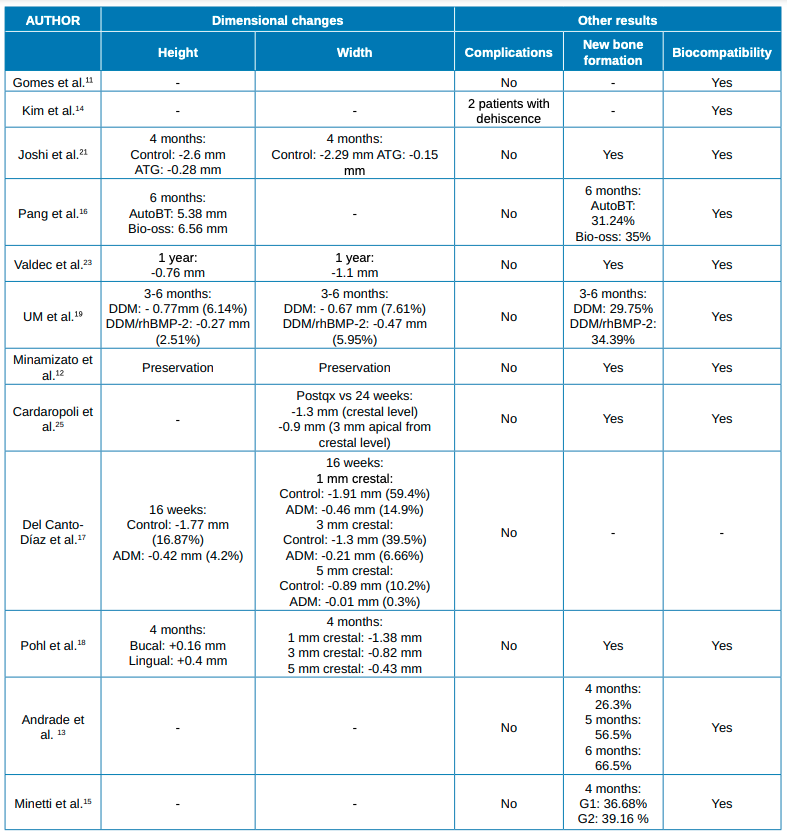
Introduction: The biological processes that take place following dental extractions cause defects in the soft and hard tissues of the jaw, which hinder rehabilitation techniques with implants. Alveolar preservation procedures have been proposed to decrease these dimensional changes. Although autogenous bone is considered the material with the best properties, it also leads to an increase in patient morbidity. Therefore, the tooth itself is considered as an alternative. The objectives of this review were to analyse the dimensional changes in alveolar ridge height/width after alveolar preservation procedures using particulate dentin, as well as possible intraoperative and postoperative complications, new bone formation and re-entry time in the grafted area.
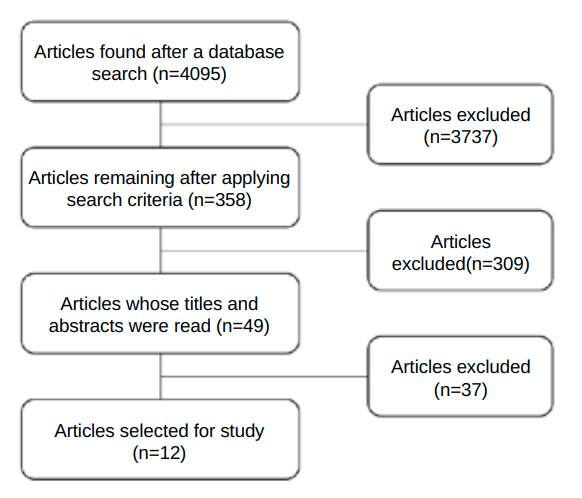
Materials and method: A review of the relevant literature in the PubMed and MEDLINE databases was carried out, identifying studies evaluating alveolar preservation procedures with particulate dentin in human patients with recorded follow-up.
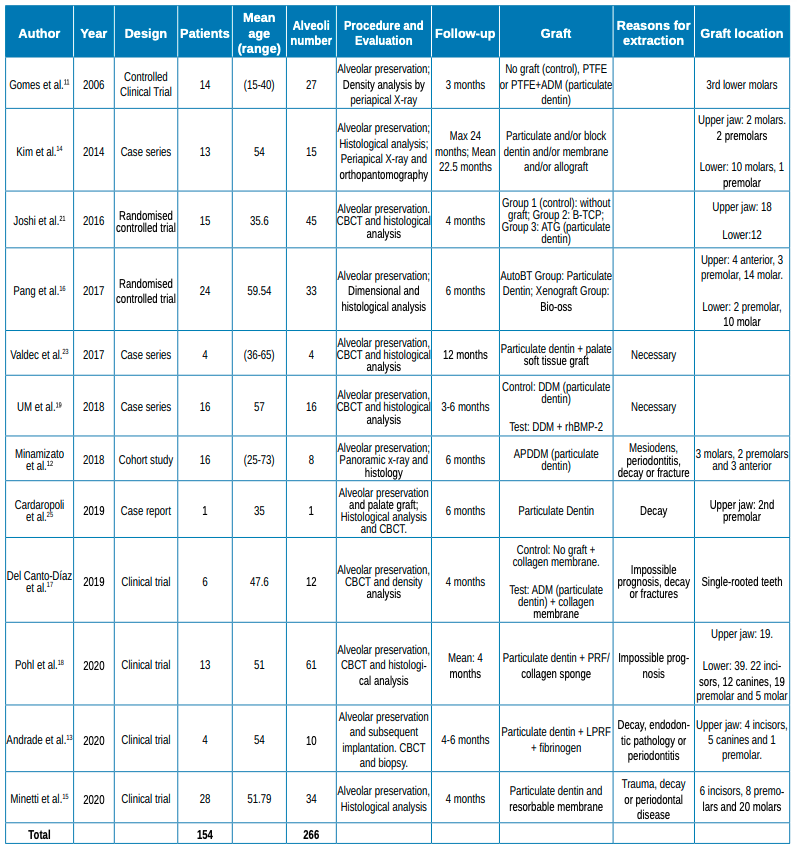
Results: A total of 12 studies were included in the systematic analysis. The dimensional changes, after grafting with particulate dentin, were comparable to those of other biomaterials and fewer than in the control groups. The occurrence of complications was low. New bone formation and re-entry time were similar to other biomaterials.
Maxillary bones are delicate structures subject to reabsorption processes, which can cause defects and limit implantological rehabilitating techniques1 . Dental extraction is one of the main reasons for these alterations in hard and soft tissue, as it can drastically modify alveolar crest volume2 . Much research has been done to evaluate the effectiveness of various biomaterials in alveolar preservation procedures. Studies in animals3 and humans4 show minor volumetric changes, despite the techniques used to prevent them. Among the biomaterials used in alveolar preservation, autogenous bone is the most predictable due to its rapid revascularisation and resistance to infection5 . However, this biomaterial also has disadvantages, such as limited availability, an increase in morbidity in the process of obtaining it and associated risks during surgery. Particulate dentin, however, is considered as an autogenous alternative with less morbidity. The results reported in the literature on this graft have been satisfactory, in vitro6 , in preclinical models in animals5,7,8 and in clinical studies in humans9,10. The objective of this review was to look at existing evidence about alveolar preservation procedures with particulate dentin.
Jung RE, Philipp A, Annen BM y cols. Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial. J Clin Periodontol 2013; 40: 90-8.
Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restirative Dent 2003; 23: 313-23.
Araujo M, Linder E, Wennstrom J, Lindhe J. The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. Int J Periodontics Restirative Dent 2008; 28: 123-35.
Barone A, Toti P, Quaranta A y cols. Clinical and Histological changes after ridge preservation with two xenografts: preliminary results from a multicentre randomized controlled clinical trial. J Clin Periodontol 2017; 44: 204-14.
Kim S, Kim H, Lim S. Combined implantation of particulate dentine, plaster of Paris, and a bone xenograft (Bio-Oss) for bone regeneration in rats. J Craniomaxillofac Surg 2001; 29: 282-8.
Calvo-Guirado JL, Ballester Montilla A, De Aza PN y cols. Particulated, Extracted Human Teeth Characterization by SEM– EDX Evaluation as a Biomaterial for Socket Preservation: An In Vitro Study. Materials 2019; 12, 380.
Bormann K, Suarez-Cunqueiro M, Sinikovic B y cols. Dentin as a suitable bone substitute comparable to ss-tcp–an experimental study in mice. Microvasc Res 2012; 84: 116-22.
Park SS, Kim SG, Lim SC, Ong JL. Osteogenic activity of the mixture of chitosan and particulate dentin. J Biomed Mater Res A. 2008; 87: 618-23.
Kim S, Yeo H, Kim Y. Grafting of large defects of the jaws with a particulate dentin–plaster of paris combination. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999; 88: 22-5.
Kim Y, Kim S, Byeon J, Lee H, Um I, Lim S, Kim S. Development of a novel bone grafting material using autogenous teeth. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; 109: 496-503.
Gomes MF, Abreu PP, Morosolli ARC, Araújo MM, Goulart MGV. Densitometric analysis of the autogenous demineralized dentin matrix on the dental socket wound healing process in humans. Braz Oral Res 2006; 20: 324-30.
Minamizato T, Koga T, Takashi I y cols.Clinical application of autogenous partially demineralized dentin matrix prepared immediately after extraction for alveolar bone regeneration in implant dentistry: a pilot study. Int J Oral Maxillofac Surg 2018; 47: 125-32.
Andrade C, Camino J, Nally M, Quirynen M, Martínez B, Pinto N. Combining autologous particulate dentin, L-PRF, and fibrinogen to create a matrix for predictable ridge preservation: A pilot clinical study. Clin Oral Investig 2019; 24: 1151-60.
Kim YK, Yun PY, Um IW. Alveolar ridge preservation of an extraction socket using autogenous tooth bone graft material for implant site development: prospective case series. J Adv Prosthodont 2014; 6: 521-7.
Minetti E, Giacometti E, Gambardella U y cols. Alveolar Socket Preservation with Different Autologous Graft Materials: Preliminary Results of a Multicenter Pilot Study in Human. Materials (Basel) 2020; 13(5): 1153.
Pang KM, Um IW, Kim YK, Woo JM, Kim SM, Lee JH. Autogenous demineralized dentin matrix from extracted tooth for the augmentation of alveolar bone defect: a prospective randomized clinical trial in comparison with anorganic bovine bone. Clin Oral Impl Res 2017; 27: 809-15.
Del Canto-Díaz A, De Elío-Oliveros J, Del Canto-Díaz M, Alobera-Gracia MA, Del Canto-Pingarrón M, Martínez-González JM. Use of autologous tooth-derived graft material in the post-extraction dental socket. Pilot study. Med Oral Patol Oral Cir Bucal 2019; 24: 53-60.
Pohl S, Binderman I, Tomac J. Maintenance of Alveolar Ridge Dimensions Utilizing an Extracted Tooth Dentin Particulate Autograft and PlateletRich Fibrin: A Retrospective Radiographic ConeBeam Computed Tomography Study. Materials (Basel) 2020; 13: 1083.
Um IW, Kim YK, Park JC, Lee JH. Clinical application of autogenous demineralized dentin matrix loaded with recombinant human bone morphogenetic-2 for socket preservation: a case series. Clin Implant Dent Relat Res 2019; 21: 4-10
Pelegrine AA, Da Costa CE, Correa ME, Marques Jr JF. Clinical and histomorphometric evaluation of extraction sockets treated with an autologous bone marrow graft. Clin Oral Implants Res 2010; 21: 535-42.
Joshi CP, Dani NH, Khedkar SU. Alveolar ridge preservation using autogenous tooth graft versus beta-tricalcium phosphate alloplast: A randomized, controlled, prospective, clinical pilot study. J Indian Soc Periodontol 2016; 20: 429-34.
Machtei EE, Mayer Y, Horwitz J, ZigdonGiladi H. Prospective randomized controlled clinical trial to compare hard tissue changes following socket preservation using allo- plasts, xenografts vs no grafting: clinical and histological findings. Clin Implant Dent Relat Res 2019; 21: 14-20.
Valdec S, Pasic P, Soltermann A, Thoma D, Stadlinger B, Rücker M. Alveolar ridge preservation with autologous particulated dentin-a case series. Int J Implant Dent 2017; 3:12.
Barone, A, Aldini, NN, Fini, M, Giardino, R, Calvo Guirado, JL, Covani, U. Xenograft versus extraction alone for ridge preservation after tooth removal: a clinical and histomorphometric study. J Periodontol 2008; 79: 1370-7.
Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L, Cardaropoli G. Socket preservation using bovine bone mineral and collagen membrane: a randomized controlled clinical trial with histologic analysis. Int J Periodontics Restirative Dent 2012; 32: 421-30.
Zhao L, Xu T, Hu W, Chung KH. Preservation and augmentation of molar extraction sites affected by severe bone defect due to advanced periodontitis: A prospective clinical trial. Clin Implant Dent Relat Res 2018; 20: 333-44.
Cha JK, Song YW, Park SH, Jung RE, Jung UW, Thoma DS. Alveolar ridge preservation in the posterior maxilla reduces vertical dimensional change: A randomized controlled clinical trial. Clin Oral Impl Res 2019; 30: 515-23.
Spinato S, Galindo-Moreno P, Zaffe D, Bernardello F, Soardi CM. Is socket healing conditioned by buccal plate thickness? A clinical and histologic study 4 months after mineralized human bone allografting. Clin Oral Implants Res 2014; 25: 120-6.
Milani S, Dal Pozzo L, Rasperini G, Sforza C, Dellavia C. Deproteinized bovine bone remodeling pattern in alveolar socket: a clinical immunohistological evaluation. Clin Oral Implants Res 2016; 27:295-302.
De Risi V, Clementini M, Vittorini G, Mannocci A, De Sanctis M. Alveolar ridge preservation techniques: a systematic review and meta-analysis of histological and histomorphometrical data. Clin Oral Impl Res 2015; 26: 50-68.

Fernández-Baca Cordón, Ignacio
DDS, MSc. Master’s in Oral Surgery, Implantology and Periodontics; Alfonso X El Sabio University.
De las Rivas Folqué, Teresa
DDS. Master’s student in oral surgery, implantology and periodontics; Alfonso X El Sabio University.
López-Malla Matute, Joaquín
DDS, MSc, PhD. Master’s Lecturer in Oral Surgery, Implantology and Periodontics; Department of Periodontics, Alfonso X El Sabio University.