Clinical cas
Published in spanish Científica Dental Vol. 18. Nº 2. 2021 www.cientificadental.es
The challenge of the surgical approach in the rehabilitation of an anterior sector unitary implant in a case of high aesthetic requirements; case report
Objective: Provide a detailed description of the current evidence-based clinical approach to a post-extraction implant with immediate loading and provisionalisation.
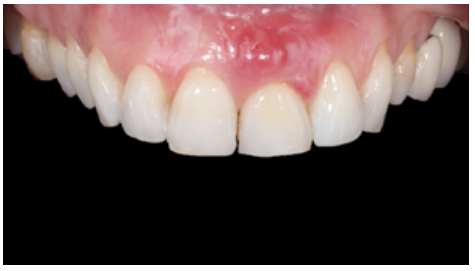
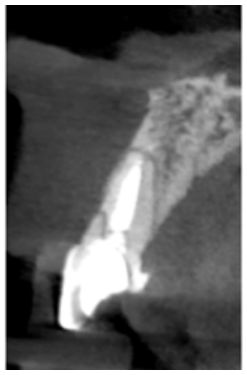
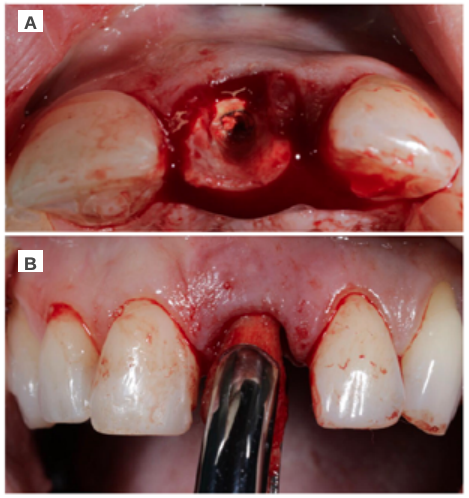
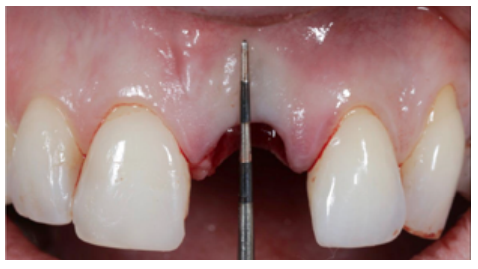
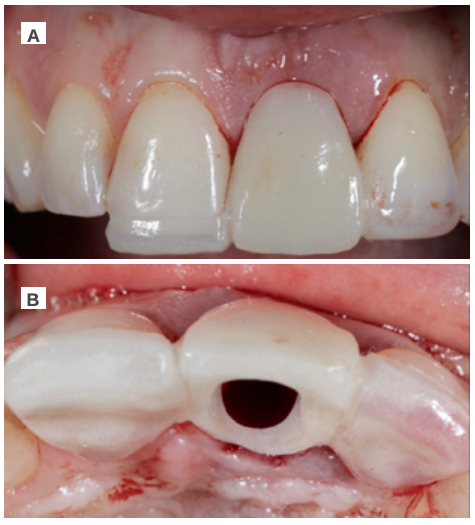
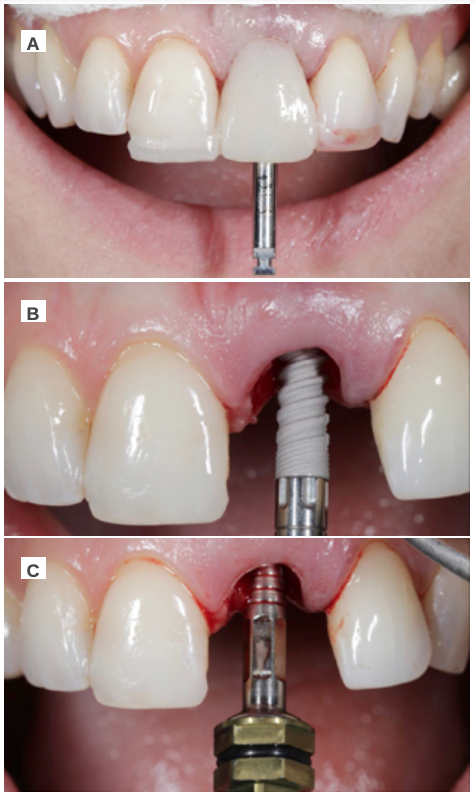
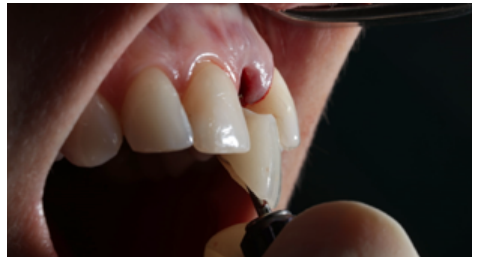
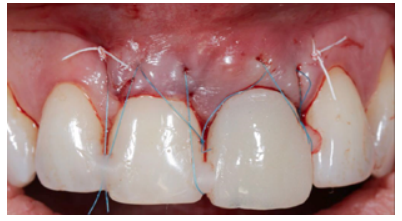
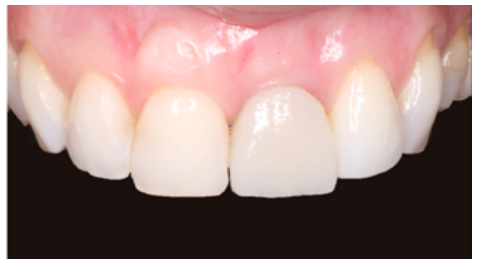
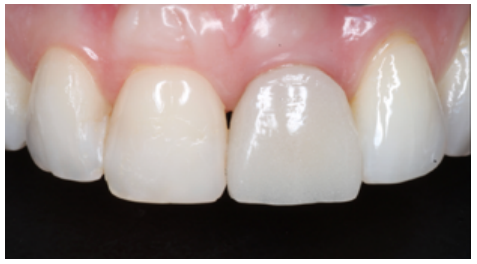
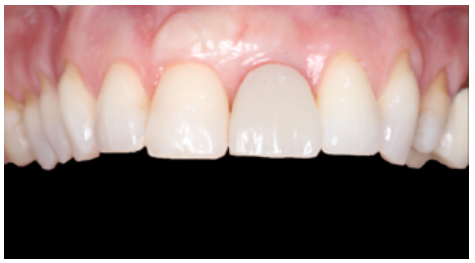
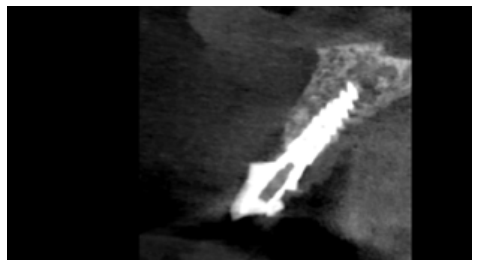
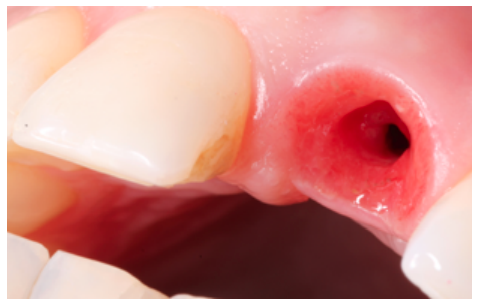
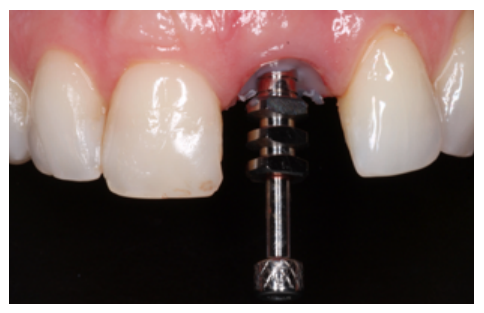
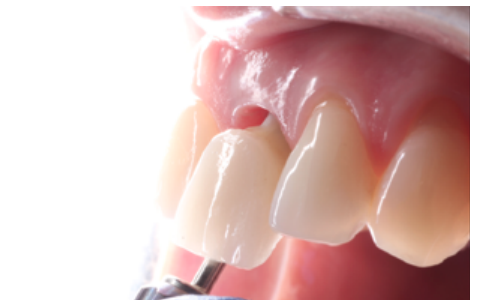
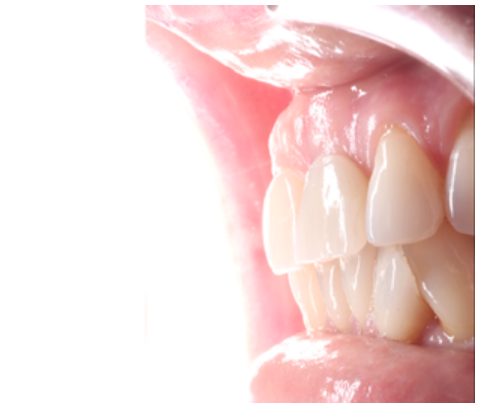
Clinical case: A 32-year-old female patient who attended for a possible root fracture of the upper left central incisor (ULCI), accompanied by a periodontal abscess at the bottom of the vestibule of the same tooth. A clinical and radiological examination established that the prognosis of the ULCI was unfavourable for conservative treatment. After evaluating the clinical features of the case, the treatment plan to extract the ULCI followed immediately by an osseointegrated implant (OII) and loading of a provisional prosthesis on the implant.
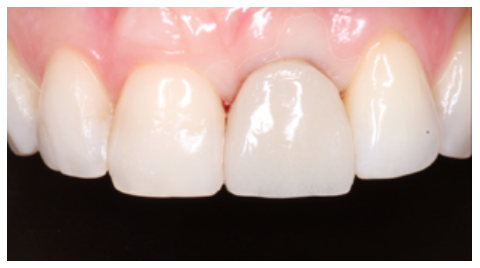
Conclusions: Rehabilitation on implants in situations of tooth loss in the aesthetic anterior sector, especially in young patients, requires a multidisciplinary treatment plan to extract the tooth and insert an OII in the correct 3-dimensional position. Various aspects need to be taken into account for this, particularly the residual remaining bone, the position of the gingival margin and preservation and conditioning of the peri-implant hard and soft tissues by means of grafts and proper handling of provisional prosthesis, until an ideal emergence profile and gingival contour is achieved before the final crown.
Oral biology has become more important in the 21st century, since it is necessary to highlight the processes related to bone and soft tissue biology, the loss of a tooth and the future of tissues after their replacement with a dental implant.
The physiological processes that take place after the extraction of a tooth are drastic, as they entail a series of modifications in the soft and hard tissues of the alveolar complex. Mainly, the microvascularisation of the architecture that surrounds the tooth suffers damage and atrophy that culminates in a decrease in the vascular supply provided by the periodontal ligament1-4. This results in a series of resorption processes discussed in this description of a clinical case.
Advances in oral implantology have brought with it new surface treatments for osseointegrated implants (OII), as well as different macroscopic designs and materials. This has been associated with greater primary stability of the OII and a better prognosis. The current trend in the field of implantology has been an evolution from conventional loading of the OII to immediate loading, due to the greater functional and aesthetic demands of society and patients5.
The benefits of immediate loading include a marked reduction in surgical interventions, less temporary dilation of the treatment and even better psychological and social wellbeing for the patient. In cases with a significant aesthetic requirement, immediate loading or provisionalisation, and post-extraction placement of the OII minimise alterations due to tooth loss and maintain the emergence profile, soft tissue contour and gingival papillae5-7.
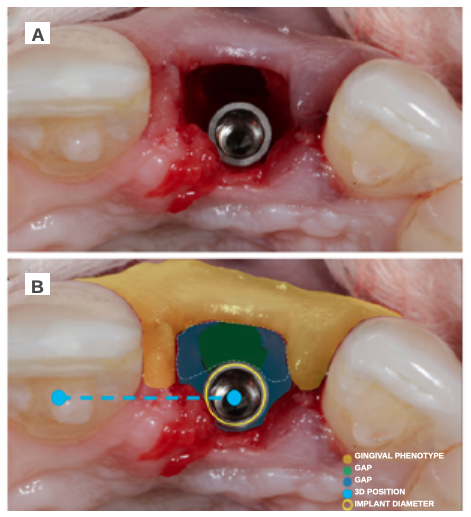
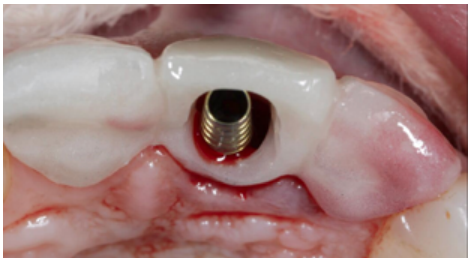
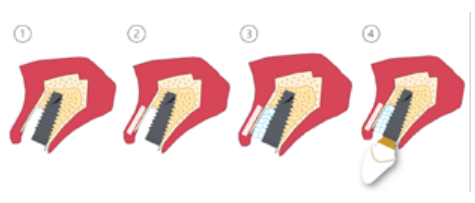
Different protocols have also been established for the management of the anterosuperior aesthetic sector, in addition to performing the immediate implant and provisional crown, including placing material between the OII and the buccal cortical to minimise possible collapse and the management of peri-implant soft tissue8-11.
The objective of this article is to provide a detailed, evidence-based description of the clinical approach to a post-extraction implant with immediate loading and provisionalisation.
Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol 2005; 32 (2): 212-8.
Araújo MG, Sukekava F, Wennström JL, Lindhe J. Ridge alterations following implant placement in fresh extraction sockets: an experimental study in the dog. J Clin Periodontol 2005; 32 (6): 645-52
Araújo MG, da Silva JCC, de Mendonça AF, Lindhe J. Ridge alterations following grafting of fresh extraction sockets in man. A randomized clinical trial. Clin Oral Implants Res 2015; 26 (4): 407-412.
Araújo MG, Sukekava F, Wennström JL, Lindhe J. Tissue modeling following implant placement in fresh extraction sockets. Clin Oral Implants Res 2006; 17 (6): 615-24.
Cheng Q, Su YY, Wang X, Chen S. Clinical Outcomes Following Immediate Loading of Single-Tooth Implants in the Esthetic Zone: A Systematic Review and Meta-Analysis. Int J Oral Maxillofac Implants 2020; 35 (1): 167-177.
Elian N, Cho SC, Froum S, Smith RB, Tarnow DP. A simplified socket classification and repair technique. Pract Proced Aesthet Dent 2007; 19 (2): 99-104.
Uribe R, Peñarrocha M, Balaguer J, Fulgueiras N. Immediate loading in oral implants. Present situation. Med Oral Patol Oral Cir Bucal 2005; 10 (2): E143-53.
Araújo M, Linder E, Wennström J, Lindhe J. The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. Int J Periodontics Restorative Dent 2008; 28 (2): 123-35.
Araújo MG, da Silva JCC, de Mendonça AF, Lindhe J. Ridge alterations following grafting of fresh extraction sockets in man. A randomized clinical trial. Clin Oral Implants Res 2015; 26 (4): 407-412.
Sanz M, Lindhe J, Alcaraz J, SanzSanchez I, Cecchinato D. The effect of placing a bone replacement graft in the gap at immediately placed implants: a randomized clinical trial. Clin Oral Implants Res 2017; 28 (8): 902-910.
Chen ST, Buser D. Clinical and esthetic outcomes of implants placed in postextraction sites. Int J Oral Maxillofac Implants 2009; 24: 186-217.
Higginbottom F, Belser R, D. Jones J, E. Keith S. Prosthetic management of implants the esthetic zone. Int. J. Oral Maxillofac Implants 2004; 19: 62-72.
Al-Sabbagh M. Implants in the Esthetic Zone. Dent Clin N Am 2006; 50: 391–407.
Buser et al. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int. J. Oral Maxillofac Implants 2004; 19: 43-61.
Buser D, Chappuis V, Belser UC, Chen S. Implant placement post extraction in esthetic single tooth sites: when immediate, when early, when late? Periodontol 2000 2017; 73 (1): 84-102.
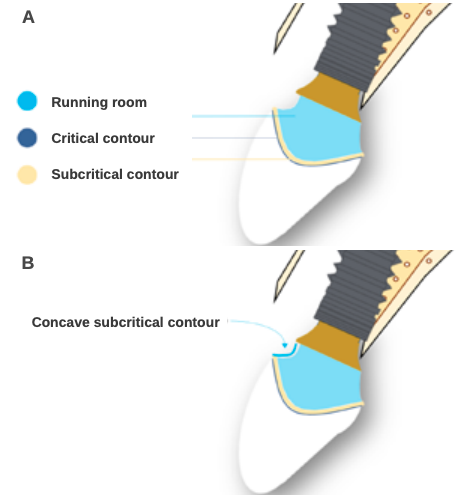
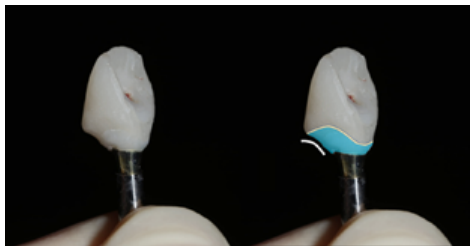
Su H, González-Martin O, Weisgold A, Lee E. Considerations of implant abutment and Crown contour: Critical contour and subcritical contour. Int J Periodontics Restorative Dent 2010; 30: 335-343
Strub JR Jurdzik BA, Tuna T. Prognosis of immediately loaded implants and their restorations: a systematic literature review. J Oral Rehabil 2012; 39 (9): 704-17.
Araújo M, Linder E, Wennström J, Lindhe J. The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. Int J Periodontics Restorative Dent. 2008; 28 (2): 123-35
Noelken R, Geier J, Kunkel M, Jepsen S, Wagner W. Influence of soft tissue grafting, orofacial implant position, and angulation on facial hard and soft tissue thickness at immediately inserted and provisionalized implants in the anterior maxilla. Clin Implant Dent Relat Res 2018; 20 (5): 674-682.
Zurh O et al. Clinical Benefits of the Immediate Implant Socket Shield Technique. J of Esthet Restor Dent 2017; 29 (2): 93-101.
Fu JH et al. Influence of tissue biotye on implant esthetics Int. J Oral Maxillofac Implants 2011; 26: 499-508.
Kan JY, Roe P, Rungcharassaeng K, Patel RD, Waki T, Lozada JL, Zimmerman G. Classification of sagittal root position in relation to the anterior maxillary osseous housing for immediate implant placement: a cone beam computed tomography study. Int J Oral Maxillofac Implants 2011; 26 (4): 873-6.
Martins-da Rosa JC, de Oliveira-Rosa AC, Fadanelli MA, Sotto-Maior B. Immediate implant placement, reconstruction of compromised sockets, and repair of gingival recession with a triple graft from themaxillary tuberosity: A variation of the immediate dentoalveolar restoration technique. Prosthet Dent 2014; 112: 717-722.
Influence of tissue biotye on implant esthetics Int. J Oral Maxillofac Implants 2011; 26: 499-508.
Olsson M, Lindhe J, Marinello CP. On the relationship between crown form and clinical features of the gingiva in adolescents. J Clin Periodontol 1993; 20 (8): 570-7.
Chapple ILC, Mealey BL, Van Dyke TE, Bartold PM, Dommisch H, Eickholz P y cols. Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup 1 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Periodontol 2018; 89 (1): S74-S84.
Papapanou PN, Sanz M, Buduneli N, Dietrich T, Feres M, Fine DH y cols. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Clin Periodontol 2018; 45 (20): S162-S170.
Müller HP, Eger T. Gingival phenotypes in young male adults. J Clin Periodontol 1997; 24 (1): 65-71.
Wennstrom JL, Derks J. Is there a need for keratinized mucosa around implants to maintain health and tissue stability? Clin Oral Implants Res 2012: 23: 136–146.
Vignoletti F, Di Domenico GL, Di Martino M, Montero E, de Sanctis M. Prevalence and risk indicators of peri-implantitis in a sample of university-based dental patients in Italy: A cross-sectional study. J Clin Periodontol 2019; 46 (5): 597-605.
Thoma DS, Mühlemann S, Jung RE. Critical soft-tissue dimensions with dental implants and treatment concepts. Periodontol 2000 2014; 66 (1): 106-18.
Bassetti RG, Stähli A, Bassetti MA, Sculean A. Soft tissue augmentation around osseointegrated and uncovered dental implants: a systematic review. Clin Oral Investig 2017; 21 (1): 53-70.